$440 billion in admin. Most of it manual.
300+ payer portals, prior auth systems, and clearinghouses — all navigated automatically, across every payer and every state.
Your Operations

Payer portals, prior auth systems, Medicaid portals, clearinghouses.

Tightrope

Record the process. AI builds, runs, and maintains it.

The Result
Fewer denials. Faster prior auth. Less rework.

What if 1 in 4 claim denials didn't trace back to eligibility errors?
70% of prior authorizations are still manual, and a denied claim costs $25 to rework. When your revenue cycle team stops doing portal work manually, your providers see more patients — without adding infrastructure costs.
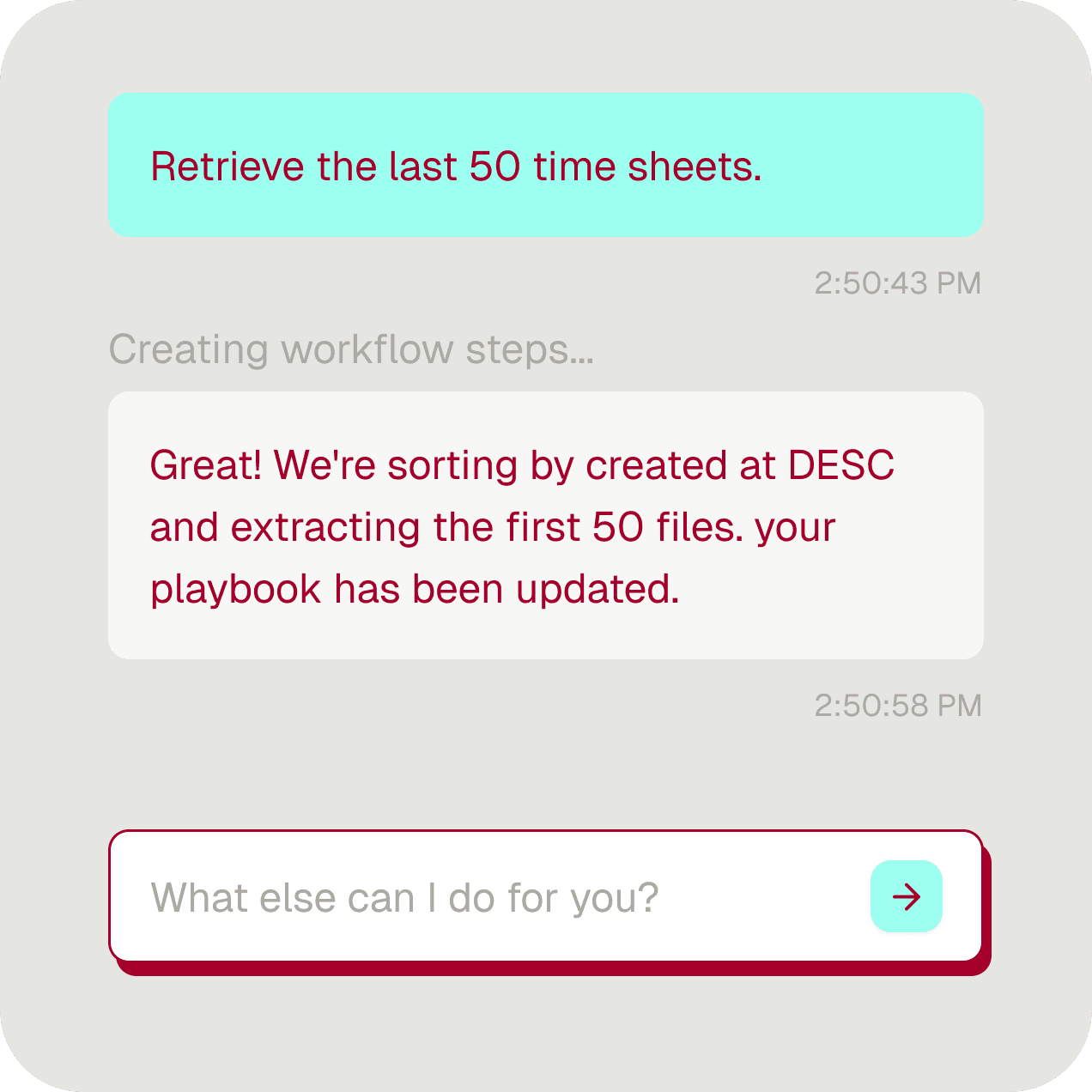
Automation discovery — as you work
Record your process once. Tightrope identifies every step, every decision point, every exception.
No process mining tool required — discovery happens when you record
Your process expert drives — no consultants documenting workflows for months
Complex auth handled for you — 2FA, SSO, rotating credentials
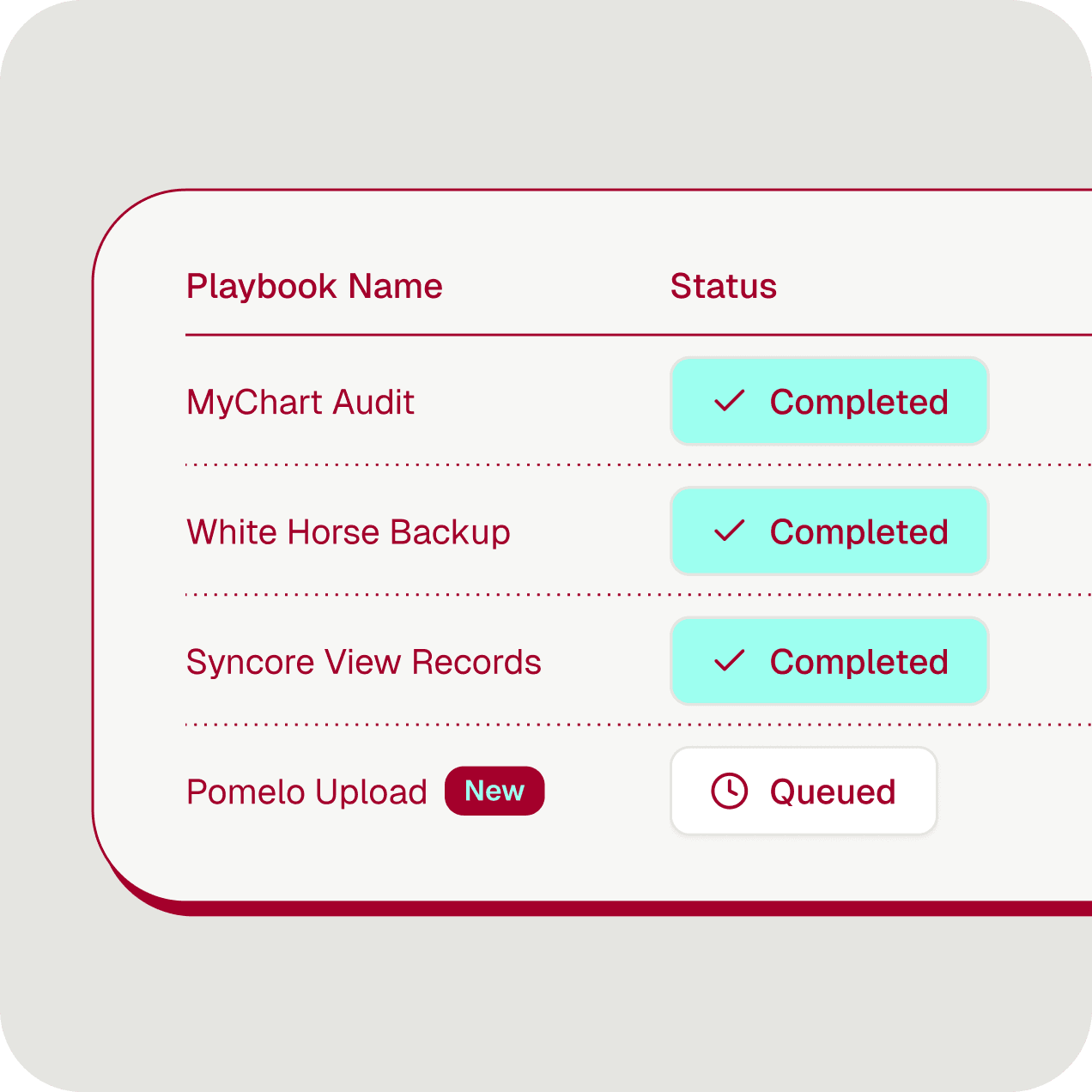
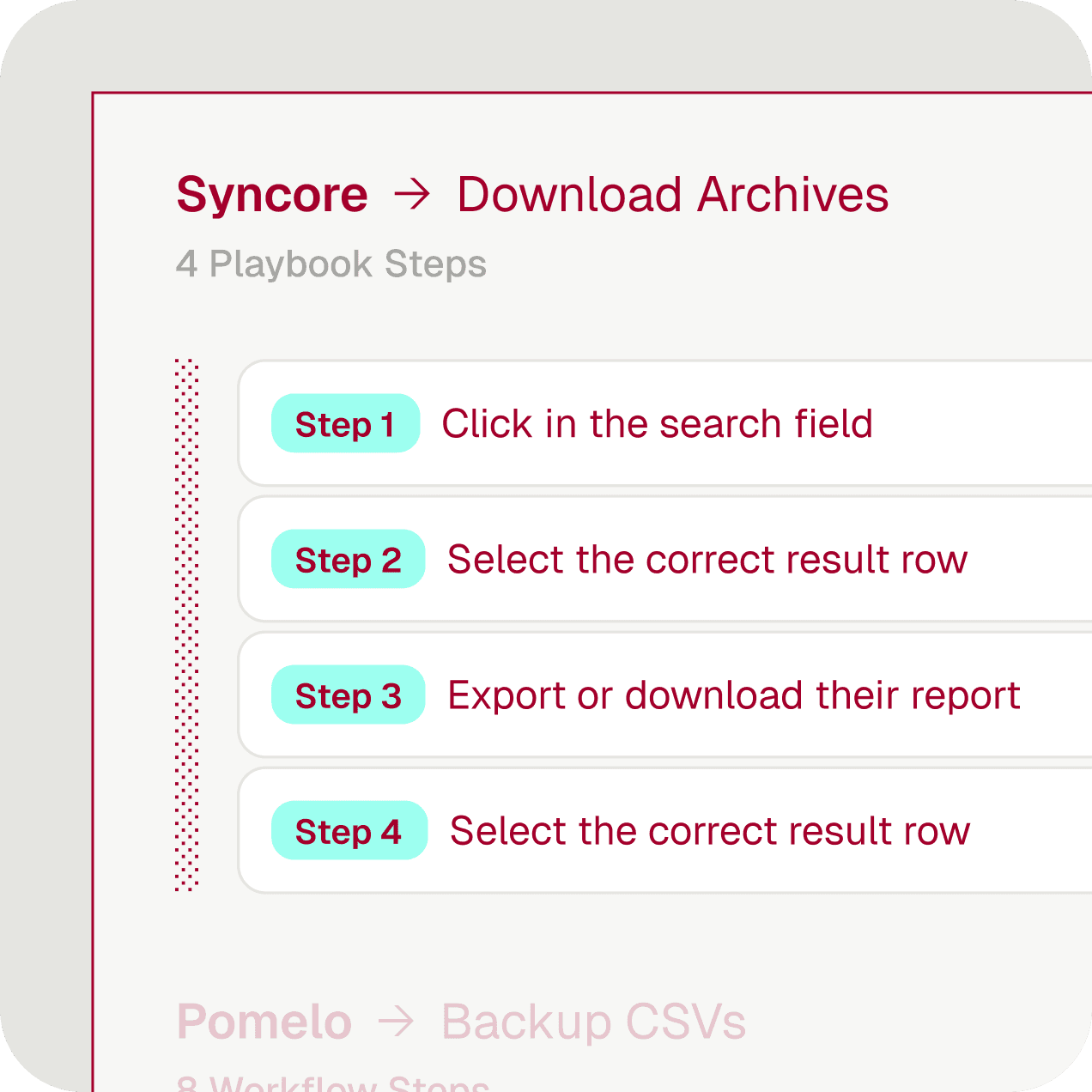
Implementation at the speed of AI
AI turns the recording into a production automation. Deploy across customers, configure per account.
Zero to 100s of workflows a year — no technical team required
One playbook, many configurations — same process, different customers
Version control and deploy — treat automations like any other codebase
Self-healing automations built for the real world
No maintenance teams. No tickets. It stays running.
Self-healing — when portals change, the automation adapts instead of breaking
Full logs and visibility — every run logged, every action replayable, audit-ready
Scales without scaling the team — five automations or five thousand, same overhead